During our 10th anniversary year, we continue to celebrate the results of our vital work, helping children in Russian clinics beat cancer, achieved with the help of our kind donors and supporters.
In June we talked to one of Russia’s leading specialists in paediatric oncology and haematology Dr. Mikhail Maschan (MD, DSc) about the difficulties of and victories in paediatric oncology and how the chances of child’s survival increase by the Power of 10 when we all work together. As Deputy Director General of the Dmitry Rogachev National Medical Research Centre in Moscow, Dr Maschan knows how crucial philanthropic support is in saving children’s lives.
Dr Maschan, it so happened that this year both the Dmitry Rogachev Centre and Gift of Life celebrate their 10-year anniversary. Over the years, most of our patients have undergone treatment for oncological and haematological diseases at your Centre, receiving support from our donors to pay for medicine, operations, and transplants. Why is this life-saving treatment covered by charitable donations and not state funding?
In Russia, treatment of cancer patients is paid for by the state at a certain tariff. This system is quite outdated; it provided high-quality treatment in 2005, but not 2021. Over the years, paediatric oncology has advanced to a great extent, and more advanced technologies have appeared that have not been considered within this outdated tariff. As such, the financial gap between the base rate and the world standard of treatment has to be covered by charities. Unfortunately, it can take years to change this tariff, as the bureaucracy extremely slows down the process.
Another issue is that the state tariff for the treatment of leukaemia, for example, is equal in both the federal centre such as Moscow and regional hospitals in smaller towns. In addition to medicines, it includes the salaries of specialists, which differ greatly by region, and the costs of operating hospital buildings, which are not comparable between clinics. For example, our Centre has a separate floor for ventilation units that ensure quality air for patients. This doesn’t exist in an ordinary regional hospital, but our tariff is standardised and calculated according to the number of patients treated.
The Rogachev Centre does not receive any additional funding. However, we don’t limit ourselves when it comes to choosing the necessary treatments, we always set high standards to try and save those patients who could not be cured previously. This requires freedom outside the scope of the national standard: the ability to move forward, buy new, more effective medicines, and introduce innovative treatment methods. And this is only possible with the help of our donors. Even in developed countries, significant progress is often driven by philanthropic funding rather than government tariffs.
And yet why, with all its resources, is Russia unable to fully treat childhood cancer and has to turn to the support of donors from abroad?
The wealth of Russia is an illusion. We remain a middle-income country in terms of GDP per capita with modest spending on public health compared to the United States and many European nations. Of course, Russia should deal with economic problems on its own, but the division of aid into domestic and foreign aid in the field of paediatric oncology is a remnant of the past. In our Centre, children who receive medical care come not only from Russia, but also from neighbouring countries, such as Kazakhstan, Moldova, and other CIS countries. For me, a child with cancer loses their nationality. Their recovery becomes a benevolent act which transcends state borders.
It is also important to remember the charity sector is only developing in Russia and doesn’t have a long history. I hope that the well-being of people will gradually increase, and they will have an urge to be generous and build a tradition of regular giving to charities. In the meantime, Russia is 100 years behind in this capacity, and the kind support of Western philanthropists is a great example for us.

In recent years a survival rate of about 80% has been achieved within the field of paediatric oncology. How accurately does this figure reflect the situation in the country?
This is true in the largest, most advanced medical centres. My estimation is that on average, in Russia, the figure is closer to 70%. There are clinics with an indicator of 50-60%. The difficulty lies in the fact that the country does not have a mechanism for collecting full statistics on long-term survival. There is only a relatively good understanding of how many children get sick annually – that is around 4500. In order not to rely entirely on government survival statistics, last year our Centre created its own register to track recovery. In the next few years, we expect to receive clear and accurate data.
We must not forget that within this 80% there are many different diseases. For example, acute lymphoblastic leukaemia has a survival rate of up to 90-95%, but glioblastoma has a rate of 5%. This range is huge: from almost completely curable diseases to diseases which have had practically no progress in ten years. Therefore, when it comes to the chance of recovery, you need to consider the data on a specific disease.
Apart from the numbers, it’s important to understand that childhood cancer is not a death sentence. The chances of curing a child are very high if you invest effort, money, and modern technology. And it is just as important to understand that 20% of patients – every fifth child – unfortunately cannot be saved, even using every possible resource. The success in saving that 20% now depends on research and development of medical science, and not on the functionality of our healthcare.
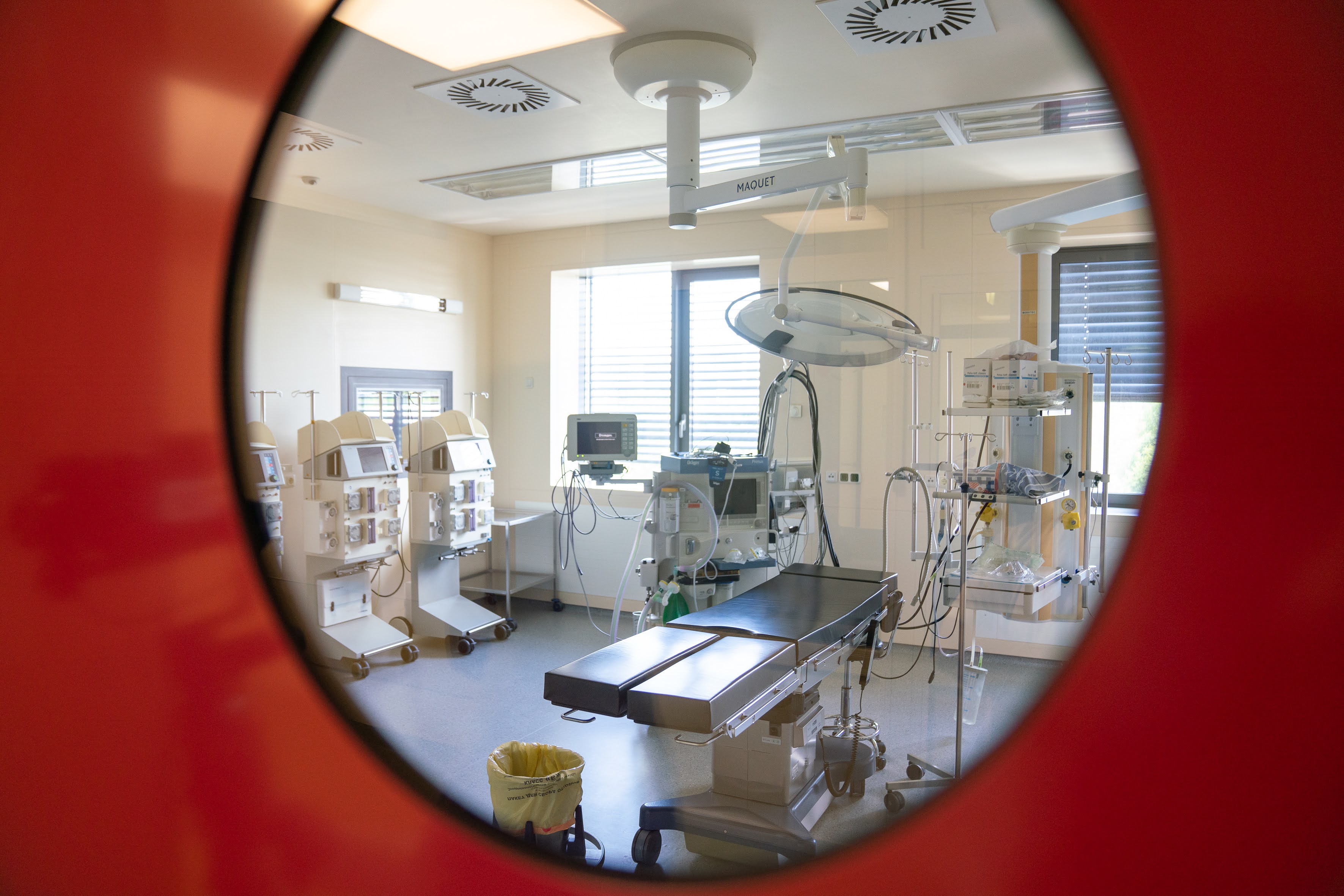
Russia lags far behind developed countries such as the United Kingdom and the United States in terms of the availability of modern onco-haematological drugs. Many medicines are simply not registered in Russia, and Gift of Life, together with its sister charities, buys them abroad. Does it so happen, then, that without the support of donors, thousands of children will be left without a chance of recovery every year?
This is largely true. It is important to understand that cancer treatment is a puzzle with hundreds of pieces. For example, in the treatment of acute lymphoblastic leukaemia, nine different anticancer drugs are used, several dozen drugs for concomitant therapy (antibiotics, antifungal and antiviral drugs, blood components), various computed tomography technologies, MRIs, ultrasounds, and more. To give a child the maximum chance at recovery, you need to put all the pieces of the puzzle in their place. The loss of even one element is detrimental to the success of the treatment.
To continue the analogy, there are simple pieces in the puzzle which are always at our fingertips; there are also very rare pieces, such as the expensive medicine Erwinase, that are unavailable in Russia, and these can only be obtained with the help of donors. It is through philanthropic support that doctors can put together the perfect puzzle for each patient.
How much does the risk of mortality increase in children who have not received effective medication on time?
If we’re talking about a patient who first fell ill with a standard tumour, then the absence of one drug from the treatment regimen can reduce the chances of recovery by several tens of percent. Take high-risk stage 4 neuroblastoma therapy. If a full treatment program is carried out with chemotherapy, radiation and transplantation, the chances of recovery are about 45%. But if you add dinutuximab immunotherapy to this combination, the chance increases to 65%. The loss of one element “kills” 20% of the success, which translates to two lives saved out of ten. That’s a lot!
There are also more radical cases. For example, with a refractory tumour, access to certain drugs or technologies, such as CAR T-cell therapy, can be a matter of life and death. With this treatment, the patient has a 50-70% chance of recovery. But without it, the chance drops to zero.

In addition to paying for medicines, Gift of Life finances the education program for Russian doctors, including specialists from your Centre. Why are professional development and continuing education so important in medicine?
Like any high-tech field, medicine is in an area of rapid growth in knowledge. Medicine is rapidly changing in 5-10 years the same way it progressed in the previous 50. If a doctor today is not informed of new procedures, he or she does not “move” medicine forward, and in ten years they become useless, not even understanding what drugs to use in treatment. And vice versa, with constant training, a doctor won’t fear that their knowledge will become outdated, and therefore they are actively practicing, saving hundreds of children’s lives.
This is the case where, “you have to run as fast just to stay in the same place”; this includes participation in international forums and conferences. They remain an indispensable mechanism for the transfer of knowledge in our profession. Without this, it is impossible to move forward together within the civilized world and create new treatment technologies so that patients in Russia receive them no later than patients in the USA or Europe. Otherwise, we risk falling to the standard of the 90s. And when the whole world begins to treat oncology with pills instead of heavy chemotherapy, our doctors will not be able to apply these technologies, because their minds will be stuck in the old ways.
Continuing the topic of relations with foreign colleagues, could you explain the importance of foreign surgeons visiting the Centre for operations, which are also paid for by Gift of Life?
The field of paediatric hematologic oncology is highly technological and depends more on the team than on a specific doctor. But surgery remains not only science but also an individual skill, close to art. The transfer of skill from hand to hand (that is, hands-on experience) is very precious. The opportunity to learn from a giant in surgery with a unique surgical technique is incredibly valuable and brings great professional happiness. Especially for the relatively young team of surgeons of our Centre. And our doctors are incredibly grateful for the opportunity to learn from these medical luminaries.
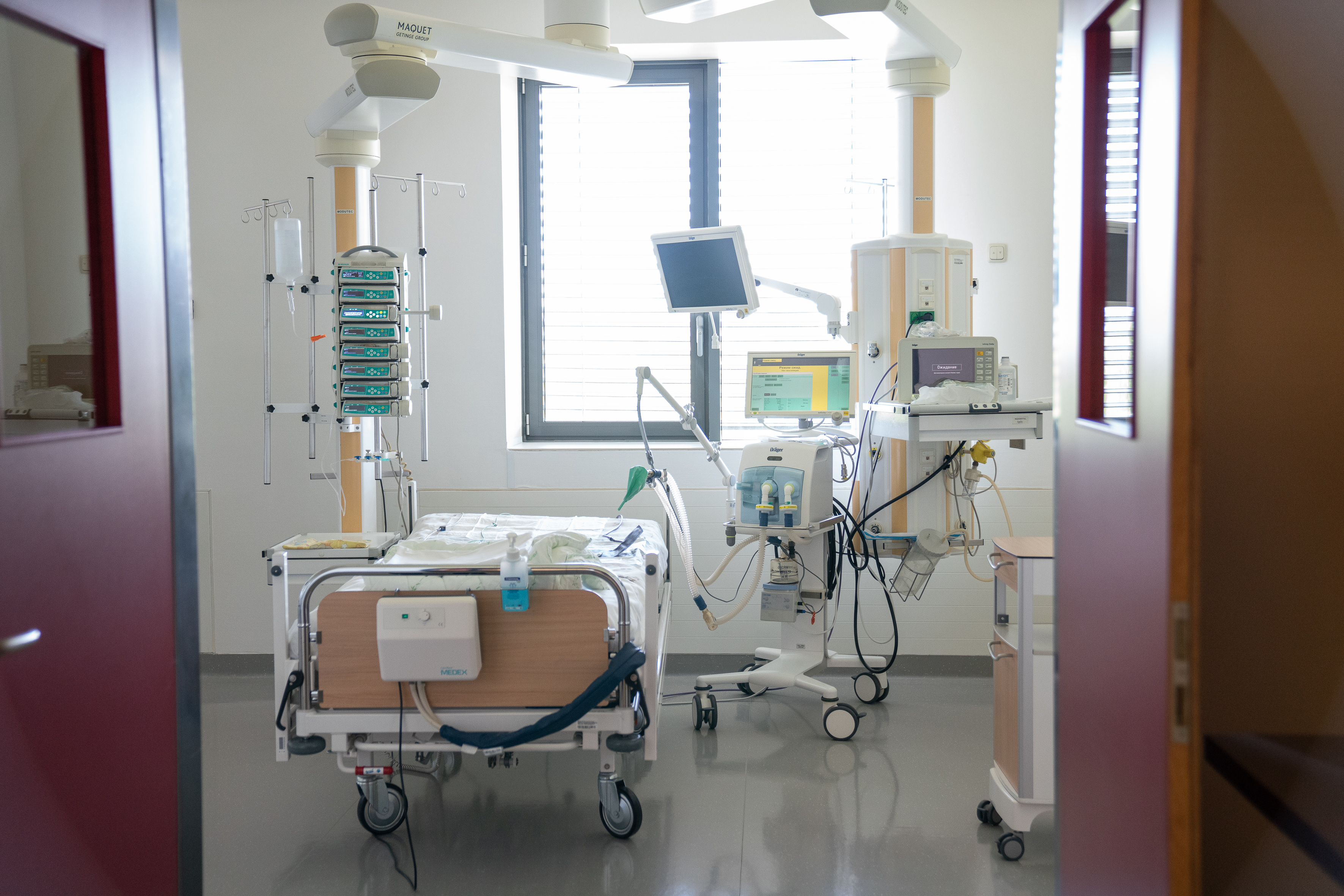
How are things going in the field of bone marrow transplantation in Russia?
Of course, there have been advancements in the past decade. With the opening of our Centre and departments of transplantation in regional children’s hospital in Yekaterinburg and the Morozov children’s city hospital in Moscow, the number of transplants in paediatrics in the country has increased by about 80%.
In Russia, about a thousand children need transplants a year. Ten years ago, we performed about 400 transplants annually, and now there are almost 700. Transplants have become more affordable, and the number of patients who try to go abroad for transplants has dropped dramatically. This is also related to the functioning of the Russian donor registry. Of course, it is still small compared to foreign ones, but even those 100,000 donors that are in it enabled many Russian transplant centres to survive this past COVID year without fatal losses. I think that in two or three years we will be able to do half of the transplants on the Russian register. In addition, everything will depend not only on the size of the register, but on the availability of rare genotypes, where the patient has one compatible donor, but that donor is, say, somewhere in Australia.
The development of transplant technologies from parents (haploidentical transplantation) also helped to keep the number of transplants at our Centre at a consistent level in 2020. We, of course, did not know that there would be a pandemic, but a few years ago we largely reoriented ourselves to parental donors. If 15 years ago everything was decided by compatibility with the donor, and the key question was “from whom” to transplant, presently new technology takes priority: every patient has a donor, we just have to decide how to make the transplant in the optimal way and on time.
COVID-19 pandemic with its travel restrictions considerably reduced availability of donors for transplants. In our Centre not more than 10-15% of patients are affected, but it is a bigger issue for some other clinics. Hopefully things will change for the better soon for everyone.
What are your expectations for the next year? In particular, from the development of cell therapy at the Centre, an area of experimental treatment that has already yielded positive results.
Our Centre actively develops cell therapy technologies and places great hope on them. Transplantation is a dangerous method of treatment associated with serious risks for the patient. But thanks to new technologies, that risk is lessened. A decade ago, “transplant-related mortality” was approximately 15%. By now we have managed to reduce this figure to 2-3% among patients with leukaemia, which previously seemed impossible. I would like to gain a foothold at this level and reduce the number of relapses. Our dream is to make the transplant 100% efficient and safe. And there are ideas on how to achieve this using cell technologies.
 Alexey and Mikhail Maschan
Alexey and Mikhail Maschan
This reduction in “transplant mortality” is a big win. And if I ask about the difficulties in your work, what is the first thing that comes to your mind?
Despite all the support of our donors, recent years have been difficult for the Centre. Several years ago charitable donations could sufficiently cover the need for treatment that was not paid for by the state, however in the last three years the cost of therapy has increased dramatically. New, more effective, safer, and more expensive medicines have appeared. And we suddenly found ourselves forced, in a sense, to choose who to treat. I dream that we will be able to change this, and everyone will be able to receive help, regardless of the cost of their therapy.
Gift of Life can collect significant sums for children’s treatments only thanks to the joint efforts of hundreds of caring people. Even £5 can change a child’s life, if there are a lot of such smaller donations which happen regularly, this is power of 10 in action. How does this support help save lives in your practice?
In our Centre, thousands of patients were able to survive only thanks to the support of donors. And these are not always people with high income. It is often small, wide-spread donations that save children. If you put our transplant programme in numbers, you get about 2,000 transplants in ten years. At a seventy percent survival rate, that is 1,400 young lives saved. And the technology that we use, an add-on to the standard therapy, covered by the state, was made available due to the generosity of ordinary donors and major philanthropists. Primarily, it was made possible thanks to the donors who have supported Gift of Life, Podari.Life, and Podari Zhizn sister charities.

The Dmitry Rogachev Centre
Cancer treatment is a gruelling marathon. What would you like to wish Gift of Life patients and their families on the way to recovery?
Once you’re on this path, you must walk it. It is incredibly important to know that you have done your best today, you will do your best tomorrow, and this is how you can achieve recovery day after day with your parents, family, and doctors, step by step.
I wish everyone who finds themselves in such a difficult situation strength and faith. We all have something to believe in: modern medicine, even if not a magic pill, but a complex and long-term treatment, still saves the majority of our patients. And we hope that in the next ten years, with the support of charity foundations like Gift of Life and caring people, we will be able to save everyone who needs our help.
#GOLpowerof10
To support the work of Gift of Life and help children and young people beat cancer, donate now.
Translation: Karina Zakharyan
Photos: Yulia Laskorunskaya / Podari Zhizn

